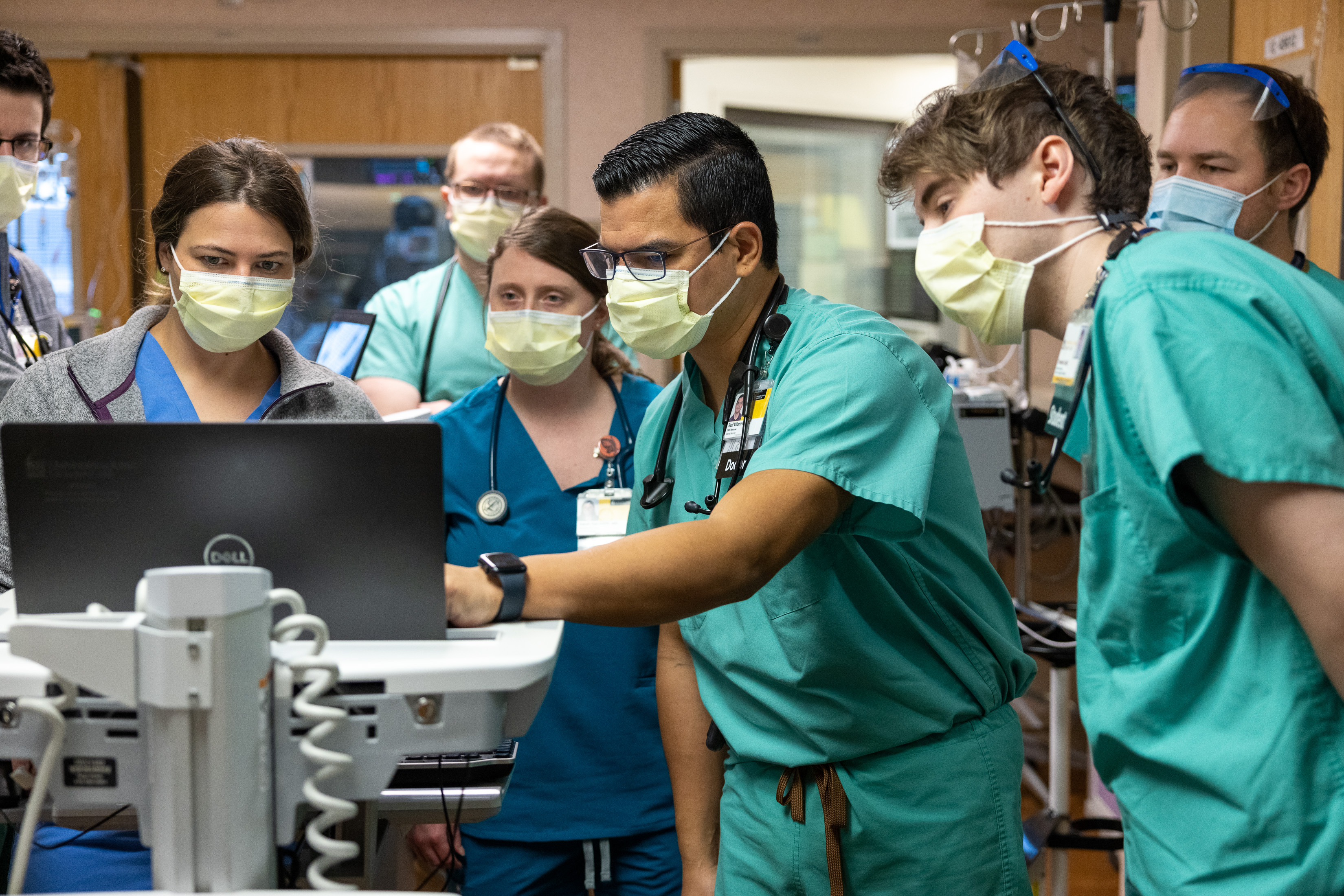
Standard safety measures for visitors, face masks now in place
April 11, 2024
8 tips to embrace the simplicity of self-care
April 1, 2024
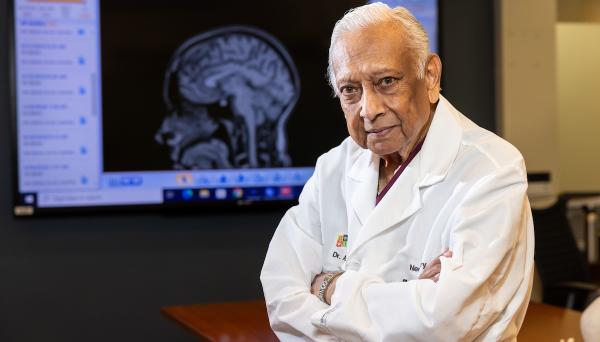
UI helping Iowa’s community hospitals improve cancer care
March 26, 2024
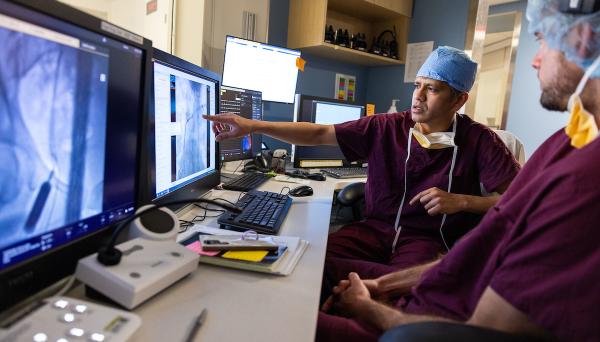
Spine surgery helps young golfer get back in the swing
March 25, 2024